Guglielmetti A, Conlledo R, Bedoya J, et al. Meditating, listening to music, going for a walk, or doing yoga are all proven ways to manage and reduce stress. Try to manage stress, as it can make psoriasis symptoms worse.Reach out to your dermatologist if psoriasis treatments irritate intimate skin areas.Use natural oils on tender skin, including olive, coconut, or emu oil.Fill the bottle with warm tap water, sit on or hover over the toilet, and gently squeeze the bottle to rinse the area after bowel movements or if you get sweaty. Rinse between showers using a bidet or peri bottle-a squeeze bottle with a narrow, angled neck.Use mild, fragrance-free cleansers on delicate skin. Take short showers using lukewarm water to avoid drying out the skin. Shower quickly so you are not leaving sweat on the body for long periods.Get plenty of fiber from your diet for easier bowel movements.Avoid getting urine or feces on the affected skin. Use good-quality toilet paper on sensitive skin to avoid causing damage to the skin and flare-ups in your intimate areas.Opt for silk, linen, and cotton options over nylon and polyester. Heavy alcohol consumption has also been linked to the development of psoriasis and a more severe disease course. Current and former smokers are at risk, but quitting smoking can bring down your risk. Smoking and alcohol consumption: Both smoking and alcohol have been linked to the development of psoriasis.This phenomenon is called Koebner’s reaction, where any skin injury-a sunburn, cut, or tattoo-can trigger psoriasis. Skin injury: Psoriasis can develop after a skin injury.Researchers think the way your immune system responds to stressors eventually leads to the chronic inflammatory response psoriasis is known for. Stress: Stress and psoriasis are linked.Both are common in people with psoriasis. Obesity: Being overweight and inactive can increase the risk of psoriasis.Medications that can lead to psoriasis include beta-blockers, lithium, nonsteroidal anti-inflammatory drugs, antibiotics, ACE inhibitors, and TNF inhibitors. Medications: Psoriasis is sometimes drug-induced.Hormones: Psoriasis affects all sexes equally, but researchers have found that female sex hormones can play a part in the development of psoriasis.It can lead to severe itchiness, dryness, and thickening of the skin. The appearance of psoriasis on the vulva is often symmetrical (affecting both sides) and appears silvery and scaly, red, or glossy red at the skin folds. In this area, psoriasis generally doesn’t affect the mucous membranes and will remain at the outer skin layers. Vulva: The vulva is external genitalia in females.This can be especially irritating when the thighs rub together with walking or running. /jock-itch-56c672f45f9b5879cc3e6623.jpg)
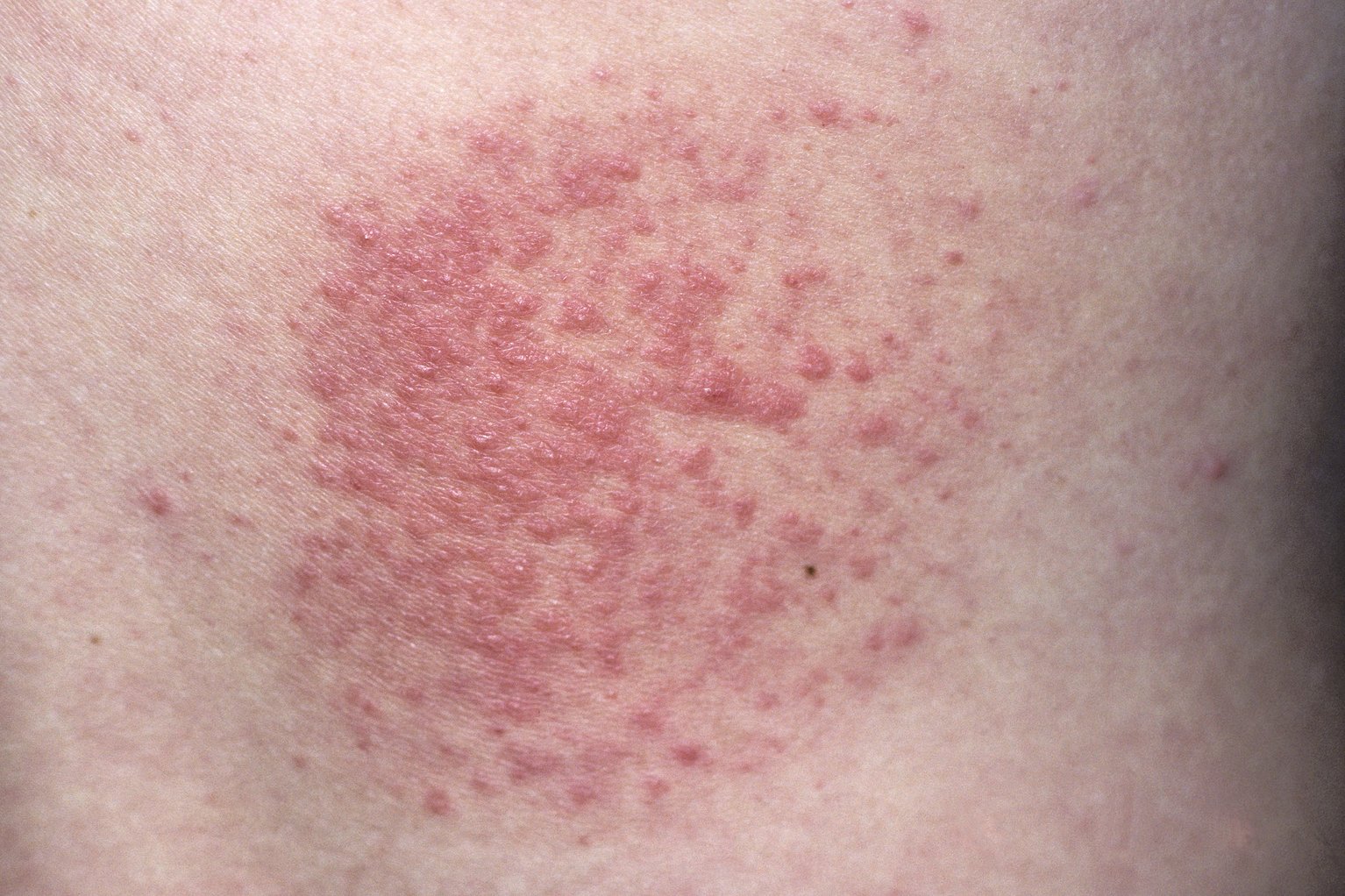
Upper thighs: Inverse psoriasis can cause red, inflamed patches on the upper thighs.Itching and scratching can make this area even more inflamed and sore. In this area, the skin is very sensitive. Pubis: The pubis, also called the pubic bone, is located just above the genitals.Psoriasis patches can be small, red, or purple and appear either scaly or smooth and shiny on the penis and scrotum. The scrotum is the sac of skin that hangs from the male body at the front of the pelvis. Penis: Psoriasis patches can show up on the penis and scrotum.People of any sex can develop inverse psoriasis at the folds between the thighs and groin. It might resemble a fungal skin infection or yeast infection. Groin and thigh fold: At the folds between the thighs and groin, psoriasis can cause the skin to crack or bleed.Buttocks: Plaque or inverse psoriasis causes itching, cracking, scaly, and bleeding skin on your buttocks or gluteal cleft.This delicate skin is more likely to get infected than psoriasis in other areas. Anus: Rashes at the anus can cause rectal bleeding and pain with passing stools.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
